1. What is the projected Compound Annual Growth Rate (CAGR) of the Medical Payment Fraud Detection?
The projected CAGR is approximately 31.1%.
 Medical Payment Fraud Detection
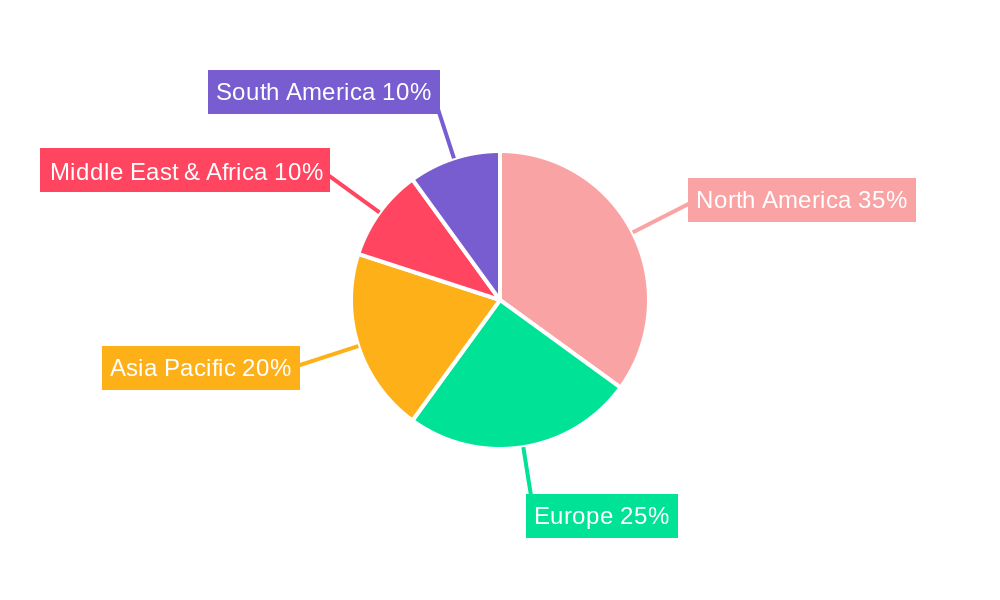
Medical Payment Fraud DetectionMedical Payment Fraud Detection by Type (On-premise, Cloud-based), by Application (Private Insurance Payers, Public/Government Agencies, Third-Party Service Providers), by North America (United States, Canada, Mexico), by South America (Brazil, Argentina, Rest of South America), by Europe (United Kingdom, Germany, France, Italy, Spain, Russia, Benelux, Nordics, Rest of Europe), by Middle East & Africa (Turkey, Israel, GCC, North Africa, South Africa, Rest of Middle East & Africa), by Asia Pacific (China, India, Japan, South Korea, ASEAN, Oceania, Rest of Asia Pacific) Forecast 2026-2034
MR Forecast provides premium market intelligence on deep technologies that can cause a high level of disruption in the market within the next few years. When it comes to doing market viability analyses for technologies at very early phases of development, MR Forecast is second to none. What sets us apart is our set of market estimates based on secondary research data, which in turn gets validated through primary research by key companies in the target market and other stakeholders. It only covers technologies pertaining to Healthcare, IT, big data analysis, block chain technology, Artificial Intelligence (AI), Machine Learning (ML), Internet of Things (IoT), Energy & Power, Automobile, Agriculture, Electronics, Chemical & Materials, Machinery & Equipment's, Consumer Goods, and many others at MR Forecast. Market: The market section introduces the industry to readers, including an overview, business dynamics, competitive benchmarking, and firms' profiles. This enables readers to make decisions on market entry, expansion, and exit in certain nations, regions, or worldwide. Application: We give painstaking attention to the study of every product and technology, along with its use case and user categories, under our research solutions. From here on, the process delivers accurate market estimates and forecasts apart from the best and most meaningful insights.
Products generically come under this phrase and may imply any number of goods, components, materials, technology, or any combination thereof. Any business that wants to push an innovative agenda needs data on product definitions, pricing analysis, benchmarking and roadmaps on technology, demand analysis, and patents. Our research papers contain all that and much more in a depth that makes them incredibly actionable. Products broadly encompass a wide range of goods, components, materials, technologies, or any combination thereof. For businesses aiming to advance an innovative agenda, access to comprehensive data on product definitions, pricing analysis, benchmarking, technological roadmaps, demand analysis, and patents is essential. Our research papers provide in-depth insights into these areas and more, equipping organizations with actionable information that can drive strategic decision-making and enhance competitive positioning in the market.
The global Medical Payment Fraud Detection market is poised for significant expansion, projected to reach approximately $12,000 million by 2025, with a robust Compound Annual Growth Rate (CAGR) of around 18% expected through 2033. This surge is primarily fueled by the escalating sophistication of healthcare fraud schemes, including billing for services not rendered, upcoding, and identity theft, which cost the industry billions annually. The increasing adoption of advanced technologies like artificial intelligence (AI) and machine learning (ML) algorithms is a key driver, enabling more accurate and efficient identification of fraudulent patterns. Furthermore, regulatory mandates and the growing emphasis on cost containment within healthcare systems are compelling payers and providers to invest heavily in robust fraud detection solutions. The shift towards cloud-based solutions is also accelerating, offering scalability, cost-effectiveness, and enhanced accessibility for a wider range of organizations.
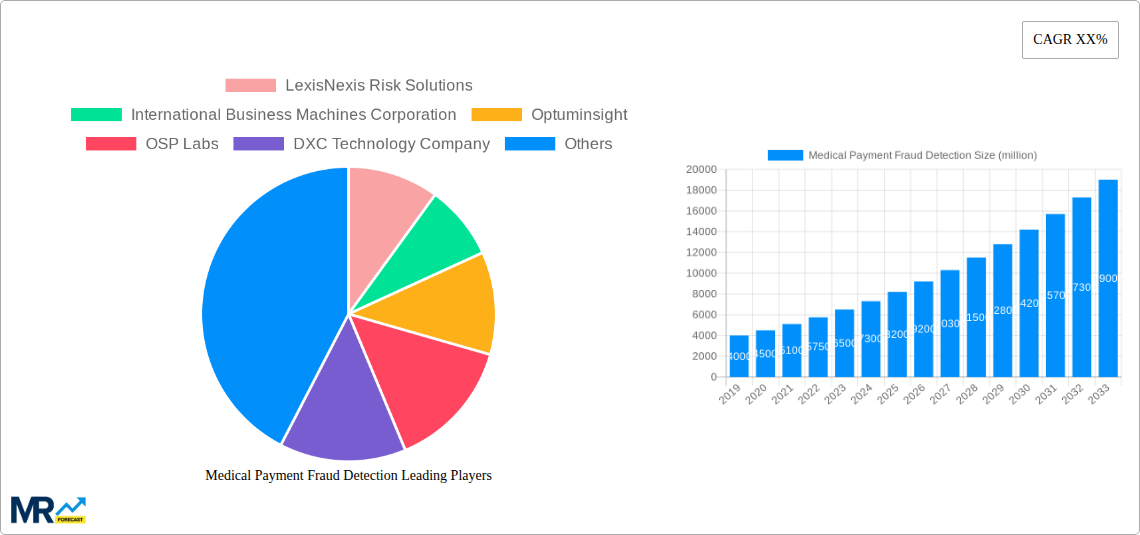

The market landscape is characterized by distinct segmentation, with "On-premise" and "Cloud-based" deployment models catering to diverse organizational needs and data security preferences. In terms of application, "Private Insurance Payers" represent a dominant segment due to the sheer volume of transactions and the direct financial impact of fraud. "Public/Government Agencies" are also significant adopters, driven by a mandate to protect taxpayer funds and ensure the integrity of public health programs. "Third-Party Service Providers" play a crucial role in offering specialized fraud detection expertise and solutions to other market players. Leading companies such as LexisNexis Risk Solutions, International Business Machines Corporation, and Optuminsight are at the forefront, driving innovation and offering comprehensive suites of tools. Geographically, North America, particularly the United States, is expected to lead the market, driven by a mature healthcare ecosystem and proactive fraud prevention initiatives. However, the Asia Pacific region is anticipated to exhibit the fastest growth, fueled by expanding healthcare access and increasing awareness of fraud-related financial losses.
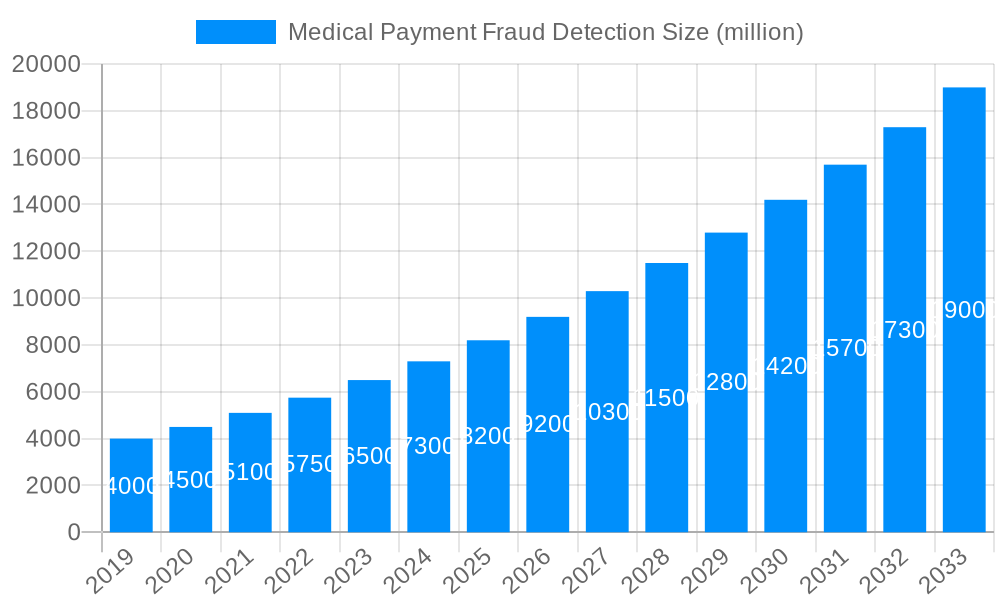

This report provides an in-depth analysis of the global Medical Payment Fraud Detection market, forecasting its trajectory from a Base Year of 2025 through to 2033. Leveraging data from the Historical Period of 2019-2024, the study meticulously examines market trends, identifies key drivers and restraints, and pinpoints dominant market segments and regions. With an estimated market size in the tens of millions and projected to reach hundreds of millions by 2033, this report offers critical insights for stakeholders navigating this rapidly evolving landscape. The analysis is structured to provide actionable intelligence, encompassing technological advancements, regulatory influences, and competitive strategies.
The global Medical Payment Fraud Detection market is experiencing a significant surge, driven by increasing healthcare expenditures and the persistent sophistication of fraudulent activities. The sheer volume of transactions and the complex billing structures within the healthcare industry create fertile ground for fraud, costing the system billions annually. XXX estimates that the market for medical payment fraud detection solutions will grow at a robust Compound Annual Growth Rate (CAGR) over the forecast period of 2025-2033. A pivotal trend is the escalating adoption of advanced analytics, including Artificial Intelligence (AI) and Machine Learning (ML), which are proving instrumental in identifying anomalous patterns and flagging suspicious claims with unprecedented accuracy. The shift towards cloud-based solutions is another dominant trend, offering scalability, cost-effectiveness, and enhanced accessibility for a wider range of healthcare organizations. This transition is further fueled by the need for real-time fraud detection capabilities, enabling payers to intercept fraudulent claims before payments are disbursed. Furthermore, there's a growing emphasis on proactive fraud prevention rather than reactive detection, with solutions increasingly incorporating predictive analytics to anticipate and mitigate potential fraud risks. The integration of big data technologies is also paramount, allowing for the analysis of vast datasets from multiple sources to build comprehensive fraud profiles. Regulatory pressures are also playing a crucial role, compelling payers to implement stringent fraud detection measures to comply with evolving legal frameworks and protect member funds. As the healthcare ecosystem becomes more interconnected, collaboration and data sharing among stakeholders, including private insurers, government agencies, and third-party providers, are becoming increasingly vital to create a unified front against fraud. The focus is shifting towards sophisticated, multi-layered detection systems that combine rule-based approaches with advanced AI/ML algorithms to combat the ever-evolving tactics of fraudsters.
Several powerful forces are propelling the growth of the Medical Payment Fraud Detection market. Foremost among these is the escalating financial burden of healthcare fraud. Estimates suggest that healthcare fraud costs the global economy billions of dollars annually, a figure that continues to climb with increasing healthcare utilization. This significant financial leakage is a primary motivator for healthcare payers to invest heavily in robust fraud detection systems. The increasing complexity of healthcare billing and coding practices, coupled with the introduction of new medical procedures and technologies, creates opportunities for intentional misrepresentation or accidental errors that can be exploited by fraudsters. Consequently, organizations require sophisticated tools to decipher these intricate billing landscapes and identify discrepancies. Moreover, the growing adoption of electronic health records (EHRs) and the digitization of healthcare processes have generated vast amounts of data. This data, while presenting privacy challenges, is also a treasure trove for fraud detection algorithms. Advanced analytics, particularly AI and ML, can process this data at scale, identifying subtle patterns and anomalies that human oversight might miss. Regulatory mandates and government initiatives aimed at curbing healthcare fraud also act as significant drivers. As governmental bodies become more aggressive in pursuing fraud, healthcare providers and payers are compelled to enhance their internal controls and invest in compliance-oriented solutions. Finally, the increasing awareness among healthcare stakeholders about the reputational damage and loss of trust associated with undetected fraud is also contributing to the market's expansion.
Despite the robust growth trajectory, the Medical Payment Fraud Detection market faces several significant challenges and restraints. One of the primary hurdles is the escalating sophistication of fraudulent schemes. As detection technologies advance, fraudsters are continuously evolving their tactics, employing more intricate methods to bypass existing safeguards. This creates an ongoing arms race, requiring constant updates and refinements to fraud detection systems. Another considerable challenge is the sheer volume and complexity of healthcare data. Integrating and analyzing diverse datasets from various sources – including claims, patient records, provider information, and external data – presents significant technical and operational complexities. This can lead to data silos and hinder the effectiveness of fraud detection algorithms. The cost of implementing and maintaining advanced fraud detection solutions can also be a restraint, particularly for smaller healthcare organizations or public agencies with limited budgets. Investing in cutting-edge technology, skilled personnel, and ongoing system maintenance requires substantial financial commitment. Data privacy and security concerns are also paramount. Handling sensitive patient information necessitates strict adherence to regulations like HIPAA, and any breach can result in severe penalties and reputational damage. Ensuring compliance while effectively sharing data for fraud detection purposes is a delicate balancing act. Furthermore, the shortage of skilled data scientists and fraud analysts with expertise in AI/ML and healthcare analytics can impede the effective deployment and utilization of advanced fraud detection tools. Finally, the inherent difficulty in distinguishing between genuine billing errors and deliberate fraudulent intent can lead to false positives, which can strain provider relationships and increase administrative overhead.
The Private Insurance Payers segment is poised to dominate the Medical Payment Fraud Detection market, driven by the sheer volume of claims processed and the significant financial stakes involved. Private insurance companies manage a vast array of health plans, encompassing millions of policyholders and processing billions of dollars in claims annually. This immense financial flow makes them prime targets for fraudulent activities, necessitating robust and proactive fraud detection mechanisms. The competitive landscape among private insurers also fuels investment in advanced technologies to mitigate losses and maintain profitability. Furthermore, private payers are often at the forefront of adopting innovative solutions, including AI-powered analytics and cloud-based platforms, to gain a competitive edge and safeguard their financial integrity. Their agile decision-making processes allow for quicker implementation of new fraud detection strategies compared to more bureaucratic public entities.
The United States is expected to remain the dominant region in the Medical Payment Fraud Detection market. This is largely attributable to the country's complex and fragmented healthcare system, which involves a multitude of private insurance payers, government programs like Medicare and Medicaid, and a vast network of healthcare providers. The substantial annual expenditure on healthcare in the U.S., estimated in the trillions of dollars, presents an immense opportunity for fraudsters. Consequently, both public and private entities are compelled to invest heavily in advanced fraud detection technologies and strategies to protect these substantial financial resources. The presence of numerous leading technology providers and innovative startups in the U.S. also contributes to its market leadership, fostering a dynamic ecosystem for the development and deployment of cutting-edge fraud detection solutions. The stringent regulatory environment in the U.S., coupled with active enforcement against healthcare fraud, further amplifies the demand for sophisticated detection capabilities.
The Cloud-based deployment model is rapidly gaining prominence and is expected to witness significant growth. This is driven by the inherent advantages of cloud computing, including scalability, flexibility, cost-effectiveness, and enhanced accessibility. Cloud-based solutions enable healthcare organizations, regardless of their size, to leverage sophisticated fraud detection capabilities without significant upfront infrastructure investments. This accessibility is particularly beneficial for smaller third-party service providers and public agencies that may have budget constraints. The ability to access and process vast amounts of data in real-time from anywhere, coupled with automatic updates and maintenance, makes cloud solutions an attractive proposition for combating the dynamic nature of healthcare fraud.
Several factors are acting as strong growth catalysts for the Medical Payment Fraud Detection industry. The relentless evolution of fraud tactics demands continuous innovation, pushing the development of more sophisticated AI and ML-powered solutions. The increasing digitization of healthcare records generates vast datasets, providing the fuel for these advanced analytics. Furthermore, growing regulatory scrutiny and government initiatives aimed at curbing healthcare fraud are compelling organizations to invest in robust detection capabilities. The global increase in healthcare spending also directly correlates with the potential financial losses due to fraud, amplifying the need for effective prevention and detection.
This report offers an exhaustive examination of the Medical Payment Fraud Detection market, providing comprehensive insights into its current state and future trajectory. Beyond market sizing and forecasting, it delves into the intricate interplay of technological advancements, regulatory landscapes, and competitive dynamics that shape the industry. The analysis encompasses key trends, driving forces, and challenges, offering a nuanced understanding of the market's evolution. Detailed segmentation by deployment type (On-premise, Cloud-based), application (Private Insurance Payers, Public/Government Agencies, Third-Party Service Providers), and geographical regions ensures a granular view of market opportunities and potential. The report highlights significant developments and the strategic initiatives of leading players, providing stakeholders with the necessary intelligence to make informed decisions and capitalize on emerging opportunities in the ever-evolving fight against medical payment fraud.

| Aspects | Details |
|---|---|
| Study Period | 2020-2034 |
| Base Year | 2025 |
| Estimated Year | 2026 |
| Forecast Period | 2026-2034 |
| Historical Period | 2020-2025 |
| Growth Rate | CAGR of 31.1% from 2020-2034 |
| Segmentation |
|
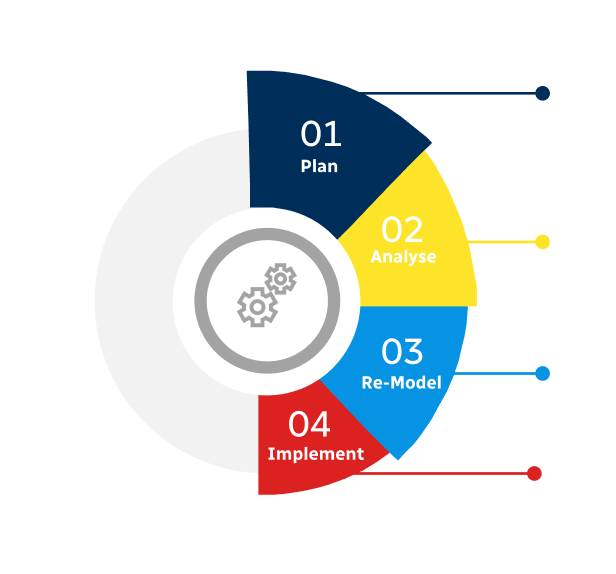
Note*: In applicable scenarios
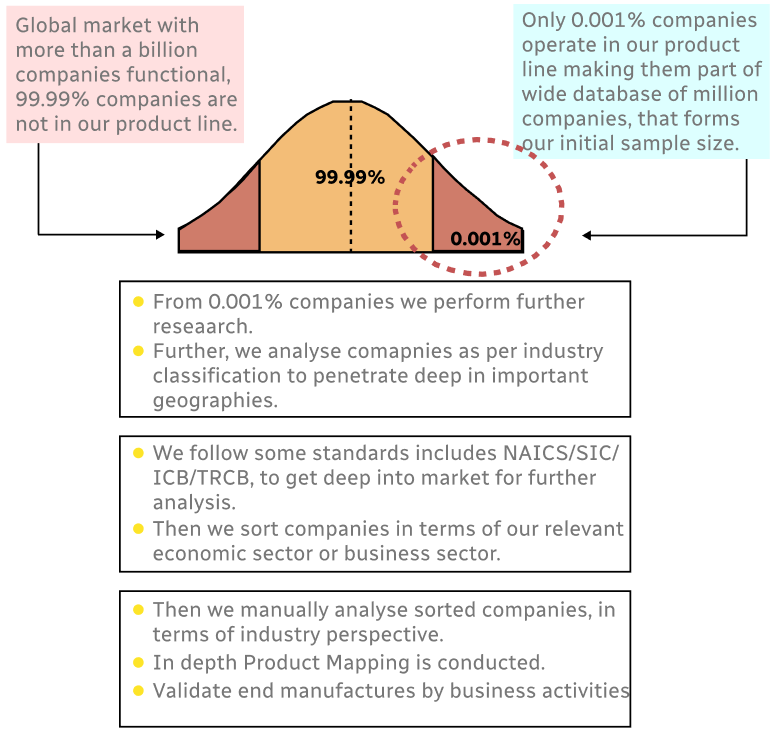
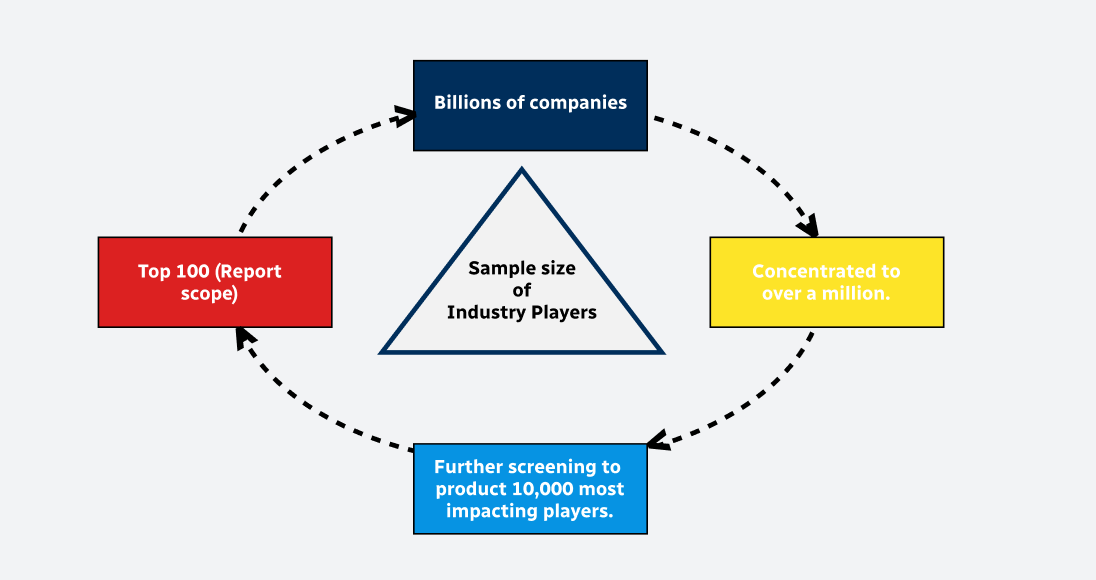
Primary Research
Secondary Research
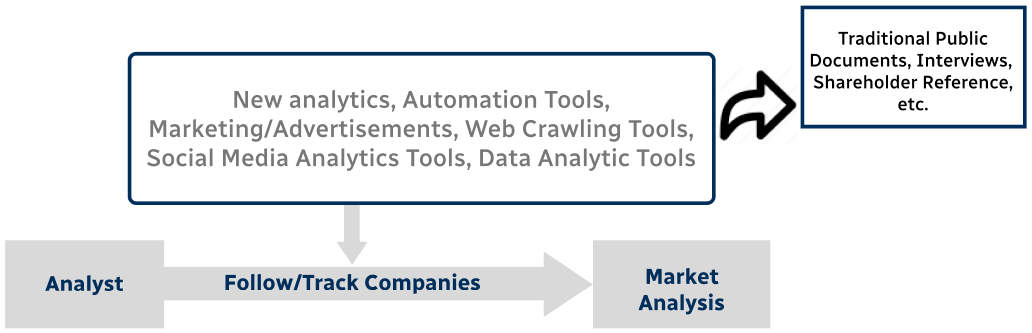
Involves using different sources of information in order to increase the validity of a study
These sources are likely to be stakeholders in a program - participants, other researchers, program staff, other community members, and so on.
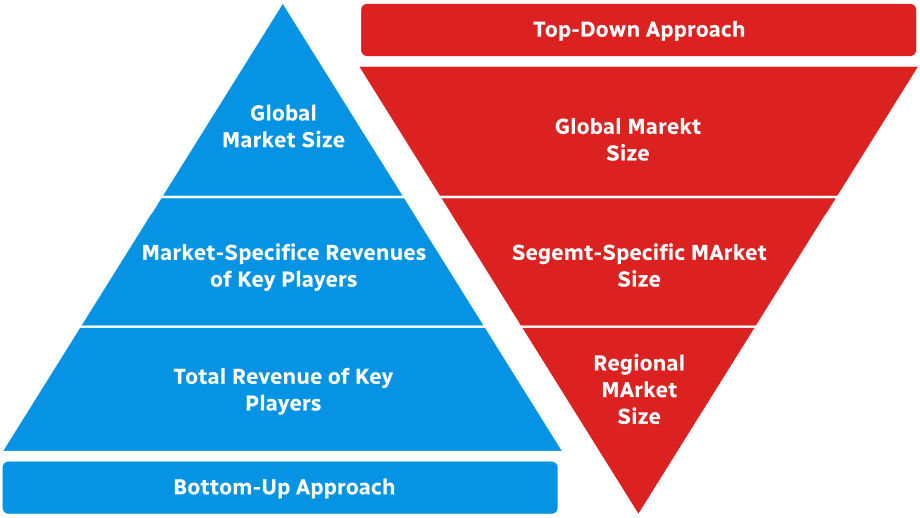
Then we put all data in single framework & apply various statistical tools to find out the dynamic on the market.
During the analysis stage, feedback from the stakeholder groups would be compared to determine areas of agreement as well as areas of divergence
The projected CAGR is approximately 31.1%.
Key companies in the market include LexisNexis Risk Solutions, International Business Machines Corporation, Optuminsight, OSP Labs, DXC Technology Company, Unitedhealth Group, SAS Institute, Fair Isaac Corporation, EXL Service Holdings, Inc., CGI GROUP, .
The market segments include Type, Application.
The market size is estimated to be USD XXX N/A as of 2022.
N/A
N/A
N/A
N/A
Pricing options include single-user, multi-user, and enterprise licenses priced at USD 3480.00, USD 5220.00, and USD 6960.00 respectively.
The market size is provided in terms of value, measured in N/A.
Yes, the market keyword associated with the report is "Medical Payment Fraud Detection," which aids in identifying and referencing the specific market segment covered.
The pricing options vary based on user requirements and access needs. Individual users may opt for single-user licenses, while businesses requiring broader access may choose multi-user or enterprise licenses for cost-effective access to the report.
While the report offers comprehensive insights, it's advisable to review the specific contents or supplementary materials provided to ascertain if additional resources or data are available.
To stay informed about further developments, trends, and reports in the Medical Payment Fraud Detection, consider subscribing to industry newsletters, following relevant companies and organizations, or regularly checking reputable industry news sources and publications.