1. What is the projected Compound Annual Growth Rate (CAGR) of the Claims Processing Software?
The projected CAGR is approximately 7.1%.
 Claims Processing Software
Claims Processing SoftwareClaims Processing Software by Type (Basic(Under $49/Month), Standard($49-89/Month), Senior($89+/Month)), by Application (Insurance Claims, Construction Claims, Injury Claims, Litigation Claims, Transportation Claims, Healthcare Claims), by North America (United States, Canada, Mexico), by South America (Brazil, Argentina, Rest of South America), by Europe (United Kingdom, Germany, France, Italy, Spain, Russia, Benelux, Nordics, Rest of Europe), by Middle East & Africa (Turkey, Israel, GCC, North Africa, South Africa, Rest of Middle East & Africa), by Asia Pacific (China, India, Japan, South Korea, ASEAN, Oceania, Rest of Asia Pacific) Forecast 2026-2034
MR Forecast provides premium market intelligence on deep technologies that can cause a high level of disruption in the market within the next few years. When it comes to doing market viability analyses for technologies at very early phases of development, MR Forecast is second to none. What sets us apart is our set of market estimates based on secondary research data, which in turn gets validated through primary research by key companies in the target market and other stakeholders. It only covers technologies pertaining to Healthcare, IT, big data analysis, block chain technology, Artificial Intelligence (AI), Machine Learning (ML), Internet of Things (IoT), Energy & Power, Automobile, Agriculture, Electronics, Chemical & Materials, Machinery & Equipment's, Consumer Goods, and many others at MR Forecast. Market: The market section introduces the industry to readers, including an overview, business dynamics, competitive benchmarking, and firms' profiles. This enables readers to make decisions on market entry, expansion, and exit in certain nations, regions, or worldwide. Application: We give painstaking attention to the study of every product and technology, along with its use case and user categories, under our research solutions. From here on, the process delivers accurate market estimates and forecasts apart from the best and most meaningful insights.
Products generically come under this phrase and may imply any number of goods, components, materials, technology, or any combination thereof. Any business that wants to push an innovative agenda needs data on product definitions, pricing analysis, benchmarking and roadmaps on technology, demand analysis, and patents. Our research papers contain all that and much more in a depth that makes them incredibly actionable. Products broadly encompass a wide range of goods, components, materials, technologies, or any combination thereof. For businesses aiming to advance an innovative agenda, access to comprehensive data on product definitions, pricing analysis, benchmarking, technological roadmaps, demand analysis, and patents is essential. Our research papers provide in-depth insights into these areas and more, equipping organizations with actionable information that can drive strategic decision-making and enhance competitive positioning in the market.
The Claims Processing Software market is experiencing robust growth, driven by the increasing need for efficient and accurate healthcare billing and reimbursement processes. The market's expansion is fueled by several key factors, including the rising adoption of electronic health records (EHRs), the increasing volume of healthcare claims, and the growing demand for improved revenue cycle management (RCM) solutions. The shift towards value-based care models also necessitates sophisticated claims processing software to manage complex reimbursement schemes and track performance metrics effectively. Furthermore, stringent regulatory compliance requirements, such as HIPAA, are driving the demand for secure and compliant software solutions. We estimate the 2025 market size to be around $10 billion, based on industry reports and observed growth trends in related software sectors. A Compound Annual Growth Rate (CAGR) of 8% is projected for the forecast period (2025-2033), indicating continued expansion.
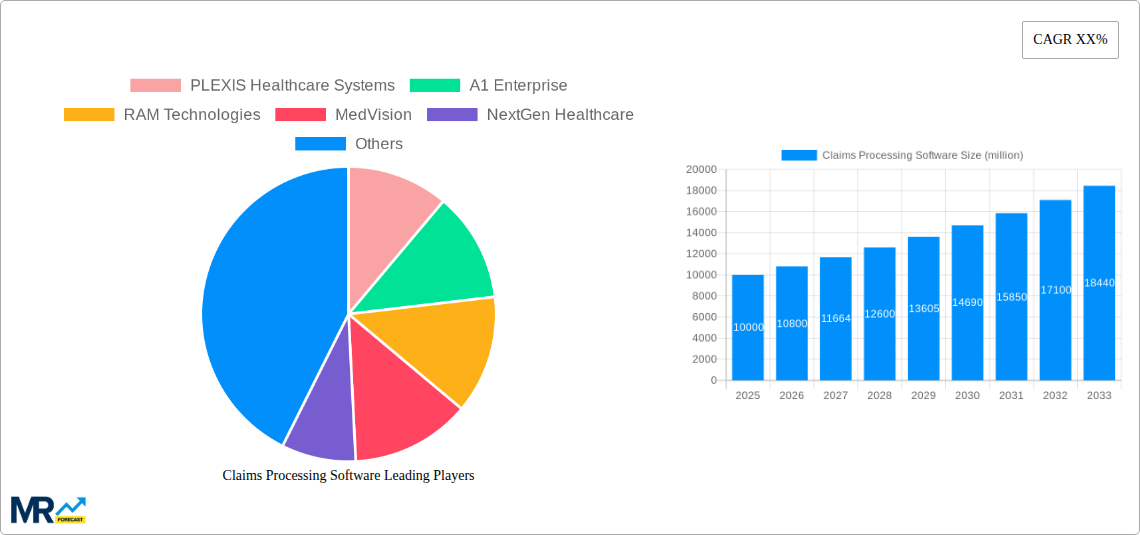

Key market segments include cloud-based solutions, which are experiencing rapid adoption due to their scalability and cost-effectiveness, and on-premise solutions which continue to hold a significant share for larger organizations prioritizing data security. Competitive rivalry is intense, with established players like NextGen Healthcare and Waystar competing with innovative smaller firms offering specialized features and streamlined workflows. While the market faces some restraints, including the high initial investment costs for implementation and the complexity of integrating software with existing systems, the overall market outlook remains positive, propelled by technological advancements and increasing regulatory pressure for improved healthcare efficiency. The market is expected to reach approximately $18 billion by 2033.
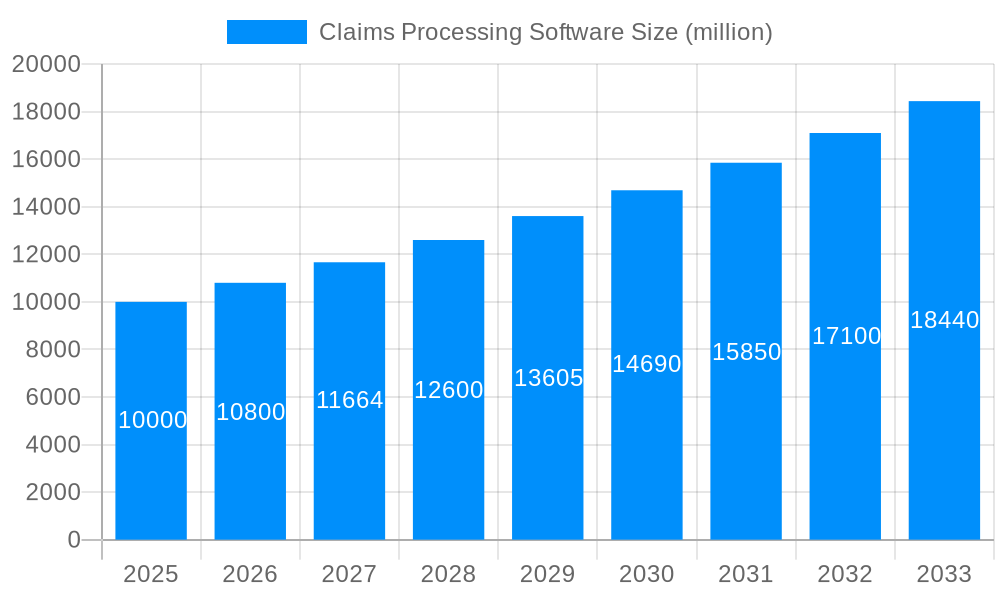

The global claims processing software market is experiencing robust growth, projected to reach multi-million unit sales by 2033. Driven by increasing healthcare data volumes, stringent regulatory compliance needs, and the escalating demand for efficient healthcare administration, the market demonstrates significant potential. The historical period (2019-2024) witnessed a steady rise in adoption, primarily fueled by the shift towards digitalization within healthcare organizations. The estimated year (2025) showcases a market already well-established, with established players consolidating their positions and new entrants focusing on niche solutions. The forecast period (2025-2033) anticipates continued expansion, propelled by technological advancements such as AI-powered automation, cloud-based solutions, and enhanced data analytics capabilities. This evolution allows for streamlined processes, reduced manual errors, and improved reimbursement rates. Furthermore, the growing emphasis on value-based care models necessitates efficient claims processing systems capable of handling complex data sets and facilitating timely payments. The integration of these systems with electronic health records (EHRs) and other healthcare IT infrastructures is a key trend, promoting interoperability and improving overall healthcare delivery. The market is witnessing a rise in the adoption of SaaS-based models, offering scalability and cost-effectiveness, particularly appealing to smaller healthcare providers. The increasing focus on patient engagement and improved patient experience also drives the market, as faster and more transparent claims processing leads to higher patient satisfaction.
Several key factors are driving the growth of the claims processing software market. The ever-increasing volume of healthcare claims necessitates automated and efficient processing systems to manage the workload effectively. Manual processing is prone to errors and delays, resulting in financial losses and decreased patient satisfaction. Claims processing software offers a solution by automating repetitive tasks, reducing errors, and speeding up the entire claims cycle. The strict regulatory environment surrounding healthcare data, particularly compliance with HIPAA in the US, necessitates software solutions capable of ensuring data security and privacy. Non-compliance can result in severe penalties, making robust security features a critical factor in software selection. Furthermore, the rising adoption of electronic health records (EHRs) creates a need for seamless integration with claims processing systems to streamline data exchange and improve workflows. This integration enables more efficient billing and reduces the administrative burden on healthcare providers. The shift towards value-based care models places increased importance on accurate and timely claims processing to ensure appropriate reimbursement and facilitate efficient healthcare delivery. Finally, the growing demand for improved patient experience pushes healthcare providers to implement solutions that speed up the claims processing cycle and enhance transparency, leading to higher patient satisfaction.
Despite its significant growth potential, the claims processing software market faces certain challenges. The complexity of healthcare regulations and compliance requirements varies significantly across different regions and countries, leading to high implementation costs and ongoing maintenance needs. Maintaining compliance with ever-evolving regulations necessitates continuous updates and adaptations of the software, adding to the financial burden. The integration of claims processing software with existing healthcare IT infrastructures can be complex and time-consuming, requiring specialized expertise and potentially disrupting existing workflows. Data security and privacy concerns are paramount in the healthcare industry, making it essential for software providers to implement robust security measures to protect sensitive patient data from breaches. The high initial investment costs associated with acquiring and implementing claims processing software can be a barrier for smaller healthcare providers with limited budgets. Finally, the lack of standardization in data formats across different healthcare systems can create interoperability challenges, hindering the seamless exchange of information and causing inefficiencies in the claims processing workflow.
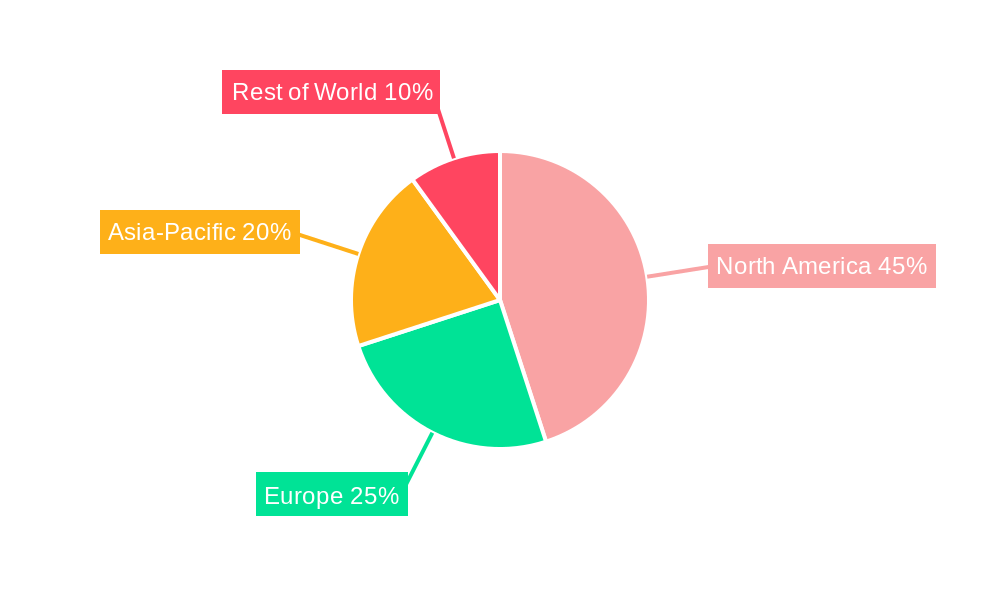
The North American market, particularly the United States, is expected to dominate the claims processing software market throughout the forecast period (2025-2033). This is due to the large and well-established healthcare industry, high adoption rates of EHRs, and stringent regulatory compliance requirements. The increasing adoption of value-based care models and the growing demand for improved patient experience also contribute to the market's dominance in this region.
High Adoption of EHRs: The widespread use of EHRs in the US creates a fertile ground for the integration of claims processing software, leading to improved workflows and reduced administrative burdens.
Stringent Regulatory Compliance: HIPAA compliance mandates robust data security and privacy measures, driving the adoption of sophisticated claims processing software solutions.
Advanced Technological Infrastructure: The mature technological infrastructure in the US supports the implementation and integration of advanced claims processing software.
Beyond North America, European markets are showing significant growth. Factors like increasing healthcare expenditure, government initiatives promoting digital healthcare, and the growing demand for efficient healthcare solutions are driving the expansion. Specific countries such as Germany and the UK are showing remarkable potential due to their relatively advanced digital healthcare ecosystems and substantial investments in healthcare IT infrastructure.
Government Initiatives: Various governmental initiatives in Europe promoting digital healthcare and interoperability are creating incentives for the adoption of claims processing software.
Increasing Healthcare Expenditure: Rising healthcare spending fuels the investment in technology solutions to optimize resource allocation and improve efficiency.
In terms of segments, the hospital segment is anticipated to dominate due to their high volume of claims processing needs and the capability to invest in advanced systems. However, the physician practice segment is poised for rapid growth, driven by the increasing number of independent practices adopting digital solutions to improve their operational efficiency.
Hospitals: High claim volumes and robust financial resources drive adoption of sophisticated, integrated systems.
Physician Practices: Increasing numbers of independent practices are seeking automation and efficiency gains.
Other Segments: Insurance companies and third-party payers will continue to need sophisticated solutions to manage increased claim volumes, contributing to market expansion within this segment.
The market’s expansion will be influenced by ongoing technological innovations, evolving regulatory landscapes, and the continuing need for improved efficiency and compliance within the healthcare sector.
The claims processing software industry is experiencing robust growth due to several key factors. The increasing volume of healthcare data necessitates automated and efficient processing, reducing manual errors and delays. Furthermore, stringent regulatory compliance requirements, like HIPAA, drive the adoption of software solutions ensuring data security and privacy. The integration of claims processing software with EHRs streamlines data exchange and improves workflows. The shift towards value-based care necessitates efficient claims processing to facilitate timely payments and optimized resource allocation. Finally, improving patient experience through faster claim processing enhances patient satisfaction and loyalty.
This report provides a comprehensive overview of the claims processing software market, offering detailed analysis of market trends, driving forces, challenges, key regions, leading players, and significant developments. The report covers the historical period (2019-2024), the base year (2025), the estimated year (2025), and the forecast period (2025-2033). It provides valuable insights for stakeholders, including software vendors, healthcare providers, and investors, enabling informed decision-making in this rapidly evolving market. The report quantifies market size in terms of millions of units, offering a granular view of segment-wise growth and regional dominance. Finally, the report includes in-depth profiles of major market participants, outlining their competitive strategies and market positions.

| Aspects | Details |
|---|---|
| Study Period | 2020-2034 |
| Base Year | 2025 |
| Estimated Year | 2026 |
| Forecast Period | 2026-2034 |
| Historical Period | 2020-2025 |
| Growth Rate | CAGR of 7.1% from 2020-2034 |
| Segmentation |
|
Note*: In applicable scenarios
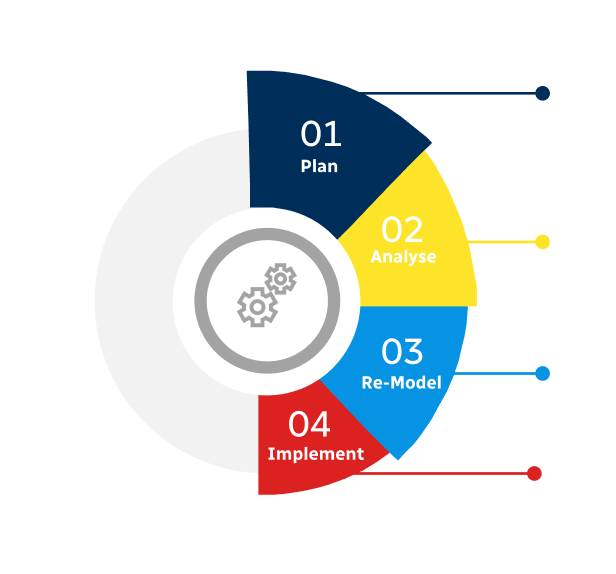
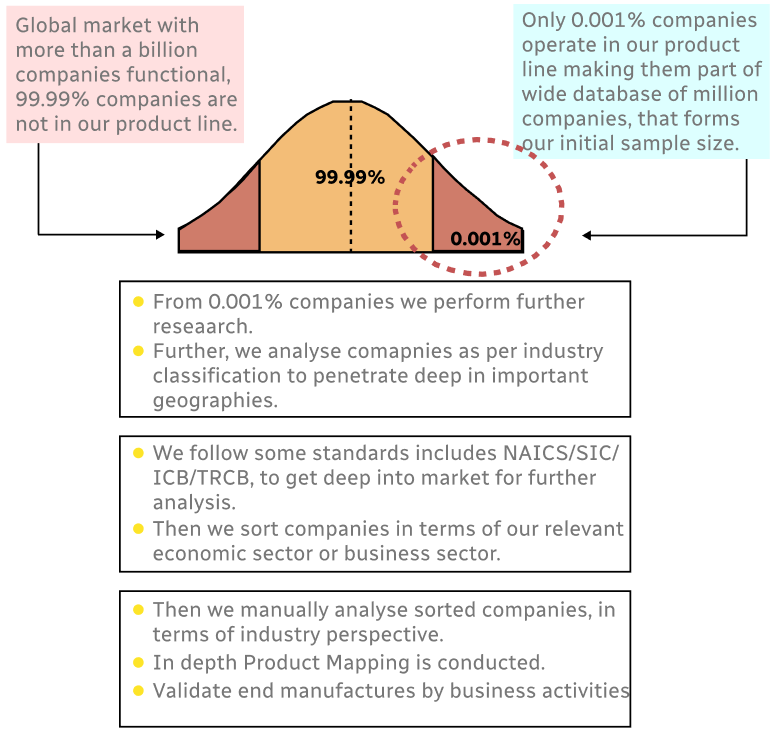
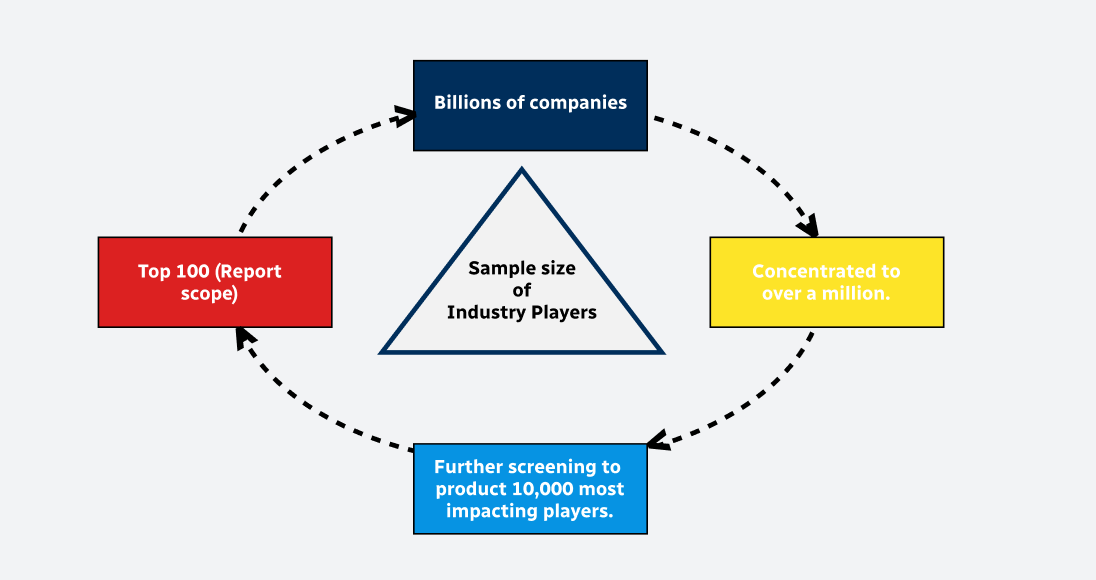
Primary Research
Secondary Research
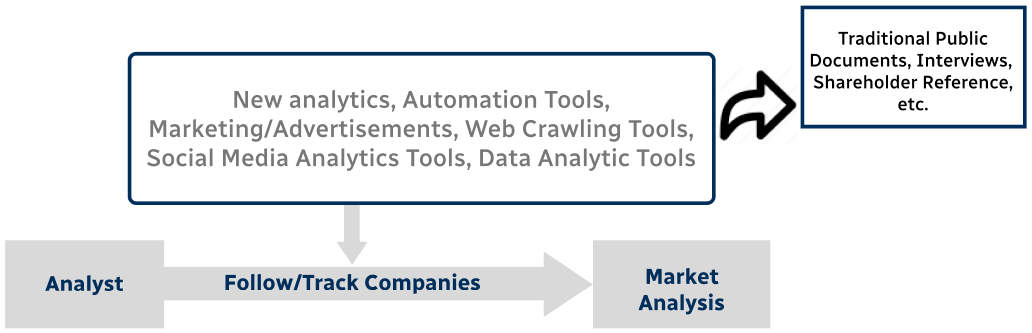
Involves using different sources of information in order to increase the validity of a study
These sources are likely to be stakeholders in a program - participants, other researchers, program staff, other community members, and so on.
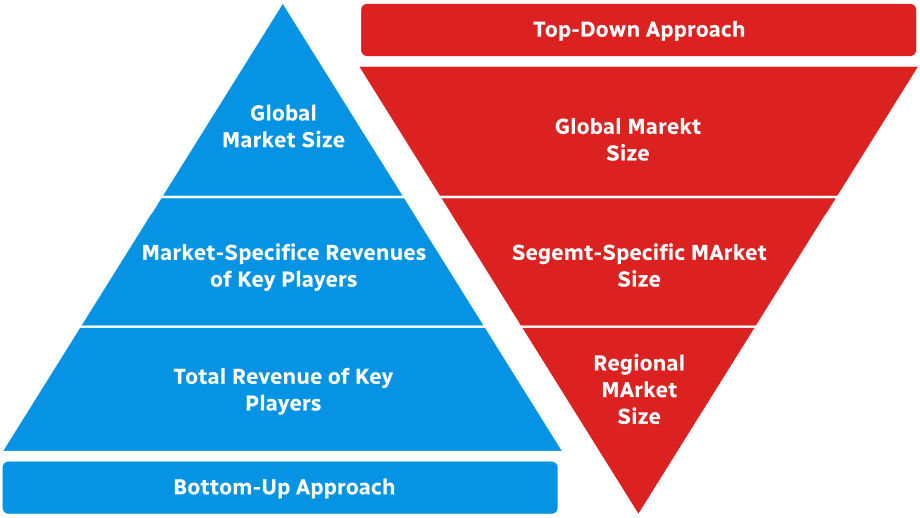
Then we put all data in single framework & apply various statistical tools to find out the dynamic on the market.
During the analysis stage, feedback from the stakeholder groups would be compared to determine areas of agreement as well as areas of divergence
The projected CAGR is approximately 7.1%.
Key companies in the market include PLEXIS Healthcare Systems, A1 Enterprise, RAM Technologies, MedVision, NextGen Healthcare, TherapyNotes, SpeedySoft USA, Drchrono, Waystar, Medical Practice Software, Meditab Software, Code Evolution, Online Reporting, ClaimLeader, DAVID, Patch, ESolutions, JW Software, Billing Dynamix, Claimable, HIPAAsuite, Mitchell International, DataCare, .
The market segments include Type, Application.
The market size is estimated to be USD XXX N/A as of 2022.
N/A
N/A
N/A
N/A
Pricing options include single-user, multi-user, and enterprise licenses priced at USD 3480.00, USD 5220.00, and USD 6960.00 respectively.
The market size is provided in terms of value, measured in N/A.
Yes, the market keyword associated with the report is "Claims Processing Software," which aids in identifying and referencing the specific market segment covered.
The pricing options vary based on user requirements and access needs. Individual users may opt for single-user licenses, while businesses requiring broader access may choose multi-user or enterprise licenses for cost-effective access to the report.
While the report offers comprehensive insights, it's advisable to review the specific contents or supplementary materials provided to ascertain if additional resources or data are available.
To stay informed about further developments, trends, and reports in the Claims Processing Software, consider subscribing to industry newsletters, following relevant companies and organizations, or regularly checking reputable industry news sources and publications.