1. What is the projected Compound Annual Growth Rate (CAGR) of the Claim Processing Software?
The projected CAGR is approximately 9%.
 Claim Processing Software
Claim Processing SoftwareClaim Processing Software by Type (/> Cloud Based, On-premises), by Application (/> Large Enterprises, SMEs), by North America (United States, Canada, Mexico), by South America (Brazil, Argentina, Rest of South America), by Europe (United Kingdom, Germany, France, Italy, Spain, Russia, Benelux, Nordics, Rest of Europe), by Middle East & Africa (Turkey, Israel, GCC, North Africa, South Africa, Rest of Middle East & Africa), by Asia Pacific (China, India, Japan, South Korea, ASEAN, Oceania, Rest of Asia Pacific) Forecast 2026-2034
MR Forecast provides premium market intelligence on deep technologies that can cause a high level of disruption in the market within the next few years. When it comes to doing market viability analyses for technologies at very early phases of development, MR Forecast is second to none. What sets us apart is our set of market estimates based on secondary research data, which in turn gets validated through primary research by key companies in the target market and other stakeholders. It only covers technologies pertaining to Healthcare, IT, big data analysis, block chain technology, Artificial Intelligence (AI), Machine Learning (ML), Internet of Things (IoT), Energy & Power, Automobile, Agriculture, Electronics, Chemical & Materials, Machinery & Equipment's, Consumer Goods, and many others at MR Forecast. Market: The market section introduces the industry to readers, including an overview, business dynamics, competitive benchmarking, and firms' profiles. This enables readers to make decisions on market entry, expansion, and exit in certain nations, regions, or worldwide. Application: We give painstaking attention to the study of every product and technology, along with its use case and user categories, under our research solutions. From here on, the process delivers accurate market estimates and forecasts apart from the best and most meaningful insights.
Products generically come under this phrase and may imply any number of goods, components, materials, technology, or any combination thereof. Any business that wants to push an innovative agenda needs data on product definitions, pricing analysis, benchmarking and roadmaps on technology, demand analysis, and patents. Our research papers contain all that and much more in a depth that makes them incredibly actionable. Products broadly encompass a wide range of goods, components, materials, technologies, or any combination thereof. For businesses aiming to advance an innovative agenda, access to comprehensive data on product definitions, pricing analysis, benchmarking, technological roadmaps, demand analysis, and patents is essential. Our research papers provide in-depth insights into these areas and more, equipping organizations with actionable information that can drive strategic decision-making and enhance competitive positioning in the market.
The claim processing software market is experiencing robust growth, driven by increasing healthcare data volumes, the need for improved efficiency in insurance claims management, and a rising adoption of cloud-based solutions. The market's expansion is fueled by several key factors: the escalating demand for faster and more accurate claim processing to reduce administrative costs and improve patient satisfaction; the increasing prevalence of electronic health records (EHRs) which necessitate integrated claim processing systems; and the growing focus on regulatory compliance, particularly HIPAA regulations in the US, driving investment in secure and compliant software solutions. The market is segmented by deployment (cloud, on-premise), functionality (claims intake, adjudication, payment), and end-user (hospitals, physician offices, insurance providers). Competition is intense among established players like ClaimLeader and Waystar, along with newer entrants offering innovative features and pricing models. The market is witnessing a significant shift towards cloud-based solutions due to their scalability, cost-effectiveness, and accessibility. This trend is projected to continue driving market growth throughout the forecast period.
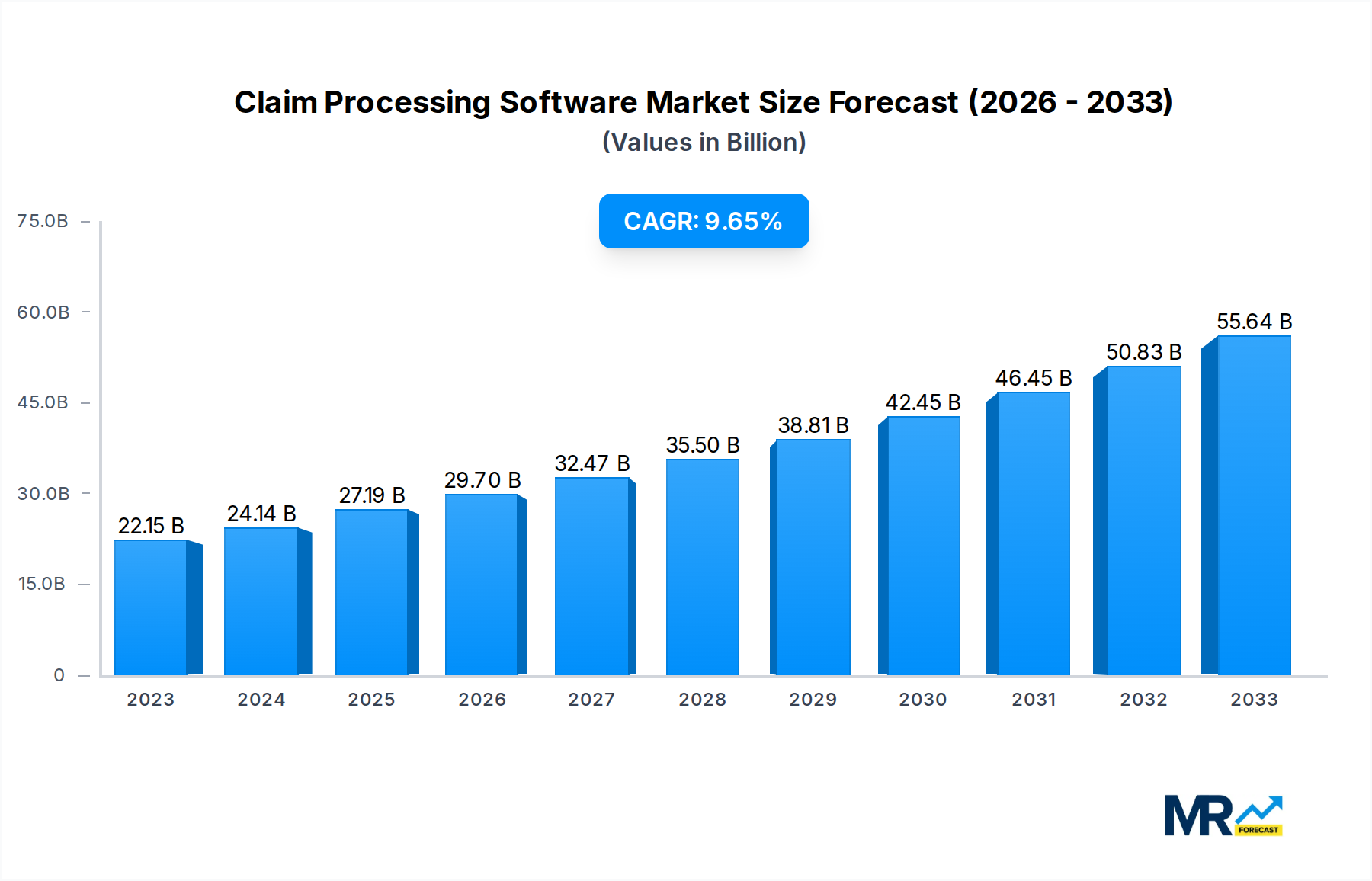

Looking ahead, market expansion is expected to be further propelled by the integration of artificial intelligence (AI) and machine learning (ML) in claim processing to automate tasks, reduce errors, and accelerate turnaround times. Furthermore, the increasing adoption of telehealth and remote patient monitoring will likely increase the volume of claims, fueling the demand for efficient claim processing software. However, challenges such as data security concerns, the high cost of implementation and integration, and the need for skilled professionals to manage and maintain these systems pose potential restraints. Despite these challenges, the long-term outlook remains positive, indicating continued substantial growth for the claim processing software market. This growth will be largely influenced by technological advancements, regulatory changes, and the evolving needs of healthcare providers and payers.
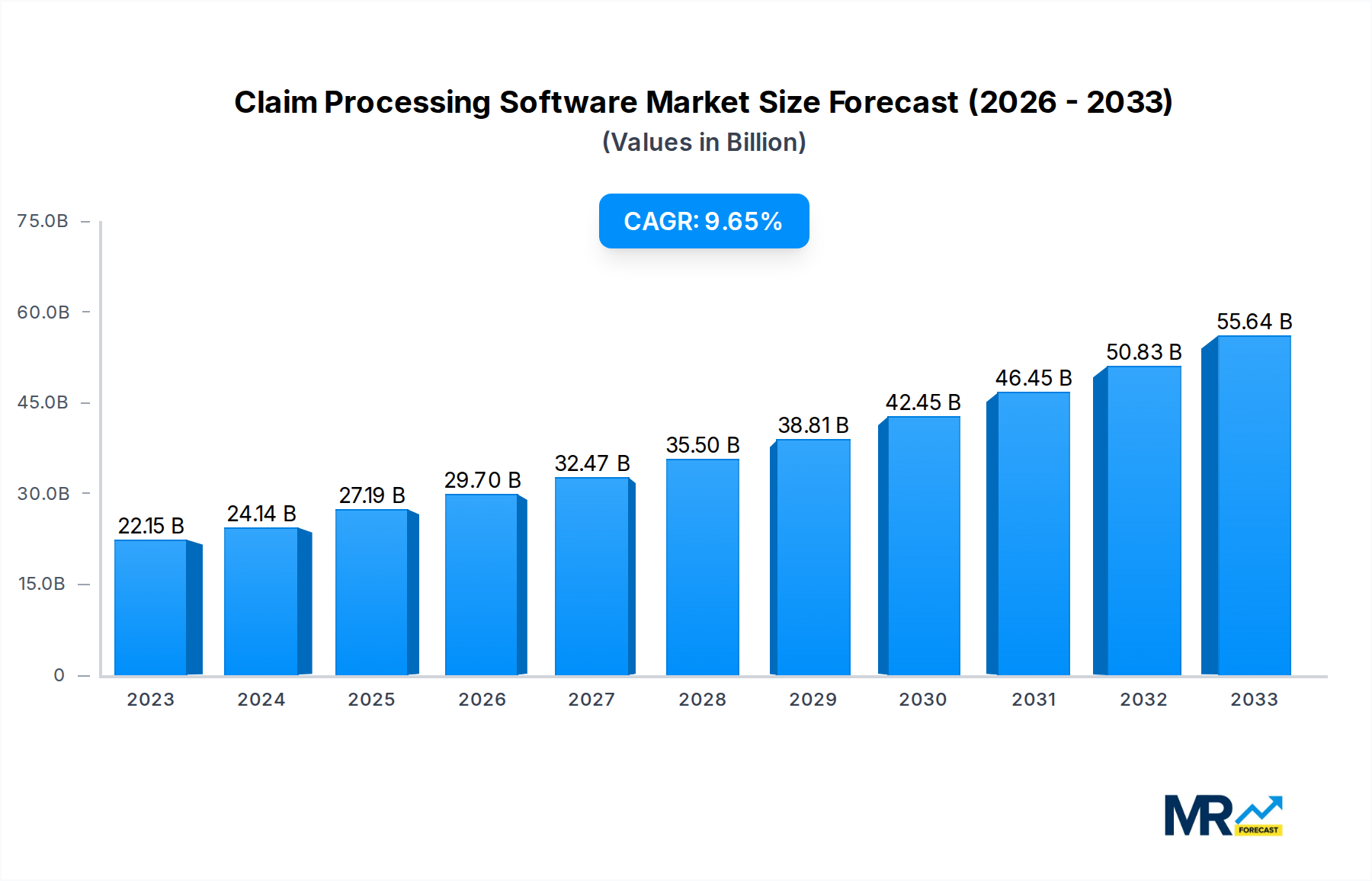

The global claim processing software market is experiencing robust growth, projected to reach multi-billion dollar valuations by 2033. Driven by the increasing need for streamlined healthcare administration and the escalating volume of insurance claims, the market has shown consistent expansion throughout the historical period (2019-2024). Key market insights reveal a strong preference for cloud-based solutions offering scalability, accessibility, and cost-effectiveness compared to traditional on-premise systems. The integration of artificial intelligence (AI) and machine learning (ML) is revolutionizing claim processing, enabling faster adjudication, reduced errors, and improved fraud detection. This technological advancement is a major trend shaping the market's trajectory, boosting efficiency and minimizing operational costs for insurance providers and healthcare facilities. The market is also seeing a rise in demand for specialized solutions catering to specific industry niches, such as dental, vision, and workers' compensation claims. Furthermore, regulatory compliance, particularly adherence to HIPAA regulations, is a significant factor driving the adoption of sophisticated claim processing software. The growing focus on enhancing patient experience and reducing administrative burdens further fuels market growth. The estimated market value in 2025 surpasses several hundred million dollars, indicating significant investment and market potential. This trend is expected to continue throughout the forecast period (2025-2033), driven by technological innovation and the increasing digitization of the healthcare industry. The shift towards value-based care models further necessitates efficient claim processing systems, accelerating the market's expansion.
Several factors are propelling the growth of the claim processing software market. Firstly, the ever-increasing volume of healthcare claims necessitates automated and efficient processing systems. Manual processing is time-consuming, prone to errors, and expensive, leading to a strong demand for software solutions that can handle large claim volumes accurately and quickly. Secondly, the rising adoption of electronic health records (EHRs) and electronic data interchange (EDI) has created an ecosystem ripe for integration with claim processing software, further streamlining workflows and reducing administrative overhead. This interoperability fosters seamless data exchange between providers, payers, and clearinghouses, minimizing delays and improving accuracy. Thirdly, the stringent regulatory environment, particularly HIPAA compliance requirements, mandates the use of secure and compliant software solutions for managing sensitive patient data. This regulatory pressure drives investment in and adoption of compliant claim processing software. Lastly, the growing focus on improving operational efficiency and reducing costs within the healthcare industry makes the implementation of cost-effective claim processing software a strategic imperative for businesses of all sizes. The cost savings associated with automation, error reduction, and improved turnaround times are significant motivators for adoption.
Despite its significant growth potential, the claim processing software market faces several challenges. Data security and privacy remain major concerns, especially given the sensitive nature of patient information handled by these systems. Maintaining compliance with evolving regulations, such as HIPAA, requires ongoing investment in security infrastructure and updates, representing a significant cost for organizations. Integration complexities can also pose a challenge, particularly when integrating with legacy systems and diverse EHR platforms. Ensuring seamless data exchange between different systems can be technically demanding and require significant IT resources. The high initial investment costs associated with implementing new software can also be a barrier to entry for smaller healthcare providers and insurance companies. Furthermore, the need for ongoing training and support to ensure effective utilization of the software adds to the overall cost and complexity. Finally, maintaining the software and adapting to changing industry standards and technological advancements necessitates ongoing investment and expertise, which can be challenging for resource-constrained organizations.
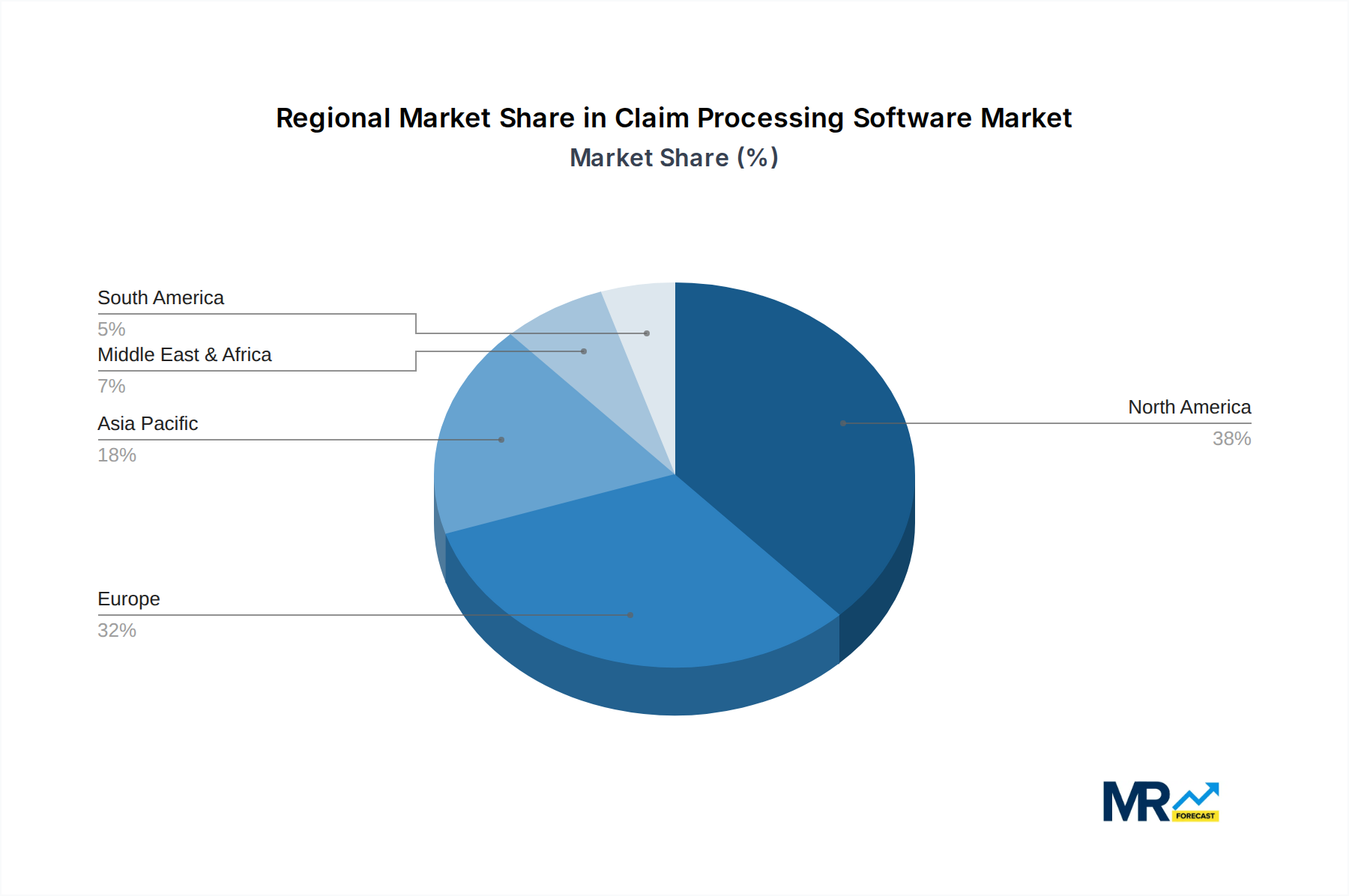
The North American market is expected to dominate the claim processing software market throughout the forecast period, driven by high healthcare expenditure, widespread adoption of EHRs, and stringent regulatory requirements. However, other regions, such as Europe and Asia-Pacific, are also experiencing significant growth, fueled by increasing healthcare investments and the growing demand for efficient healthcare administration.
Dominant Segments:
The paragraph highlights the dominance of North America, particularly the US, driven by high healthcare spending, technological advancement, and regulatory compliance requirements. The European and Asia-Pacific markets are experiencing strong growth, fueled by increasing government initiatives, rising healthcare investments, and the growing adoption of digital healthcare technologies. The cloud-based segment and large enterprise segment are also major contributors to the overall market revenue, reflecting the trend toward efficient, scalable, and compliant solutions.
Several factors are catalyzing growth within the claim processing software industry. The increasing focus on reducing administrative costs and improving operational efficiency within the healthcare sector creates a strong incentive for adopting automated solutions. The rising adoption of value-based care models necessitates efficient claim processing to track performance metrics and ensure timely payments, thereby further driving market demand. Furthermore, advancements in AI and machine learning offer enhanced capabilities for fraud detection and improved accuracy in claim adjudication, leading to cost savings and improved efficiency.
This report provides a comprehensive analysis of the claim processing software market, covering market size, trends, drivers, challenges, key players, and significant developments. The detailed insights offered within this report are valuable for businesses, investors, and researchers seeking a comprehensive understanding of this rapidly evolving market. The report's projections for the forecast period (2025-2033) provide actionable intelligence for strategic decision-making.

| Aspects | Details |
|---|---|
| Study Period | 2020-2034 |
| Base Year | 2025 |
| Estimated Year | 2026 |
| Forecast Period | 2026-2034 |
| Historical Period | 2020-2025 |
| Growth Rate | CAGR of 9% from 2020-2034 |
| Segmentation |
|
Note*: In applicable scenarios
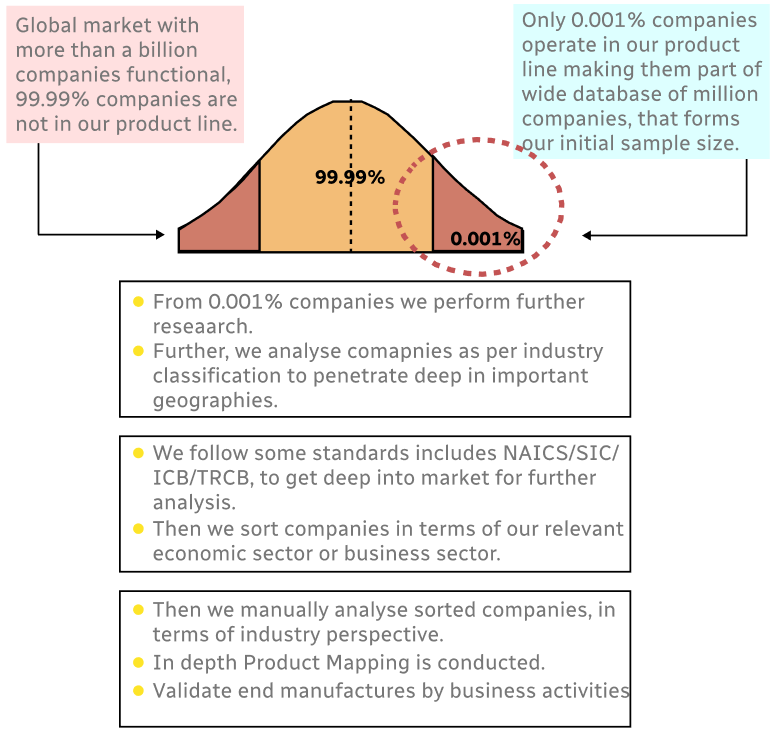
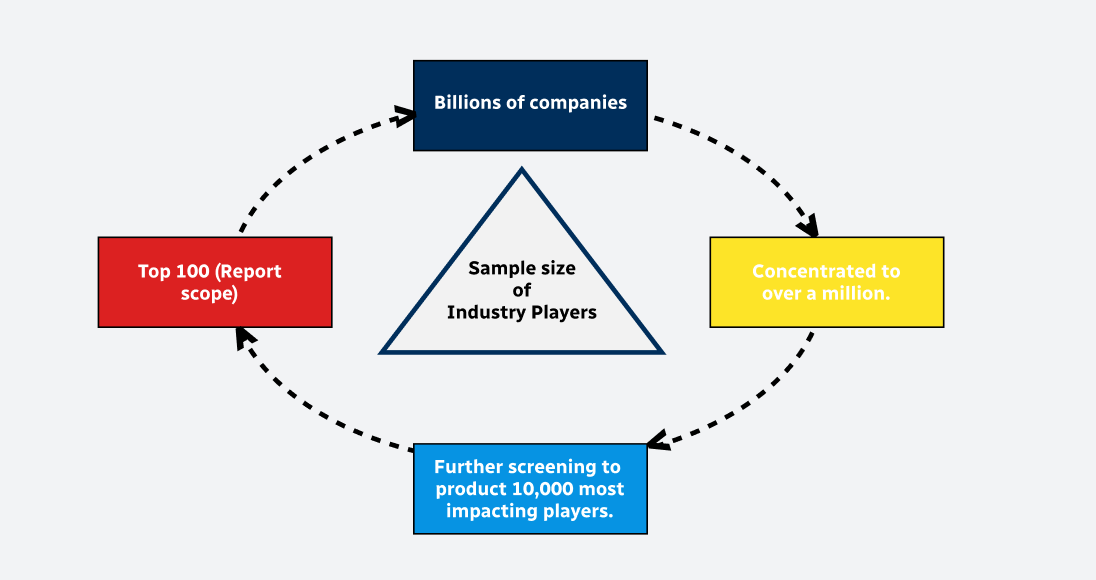
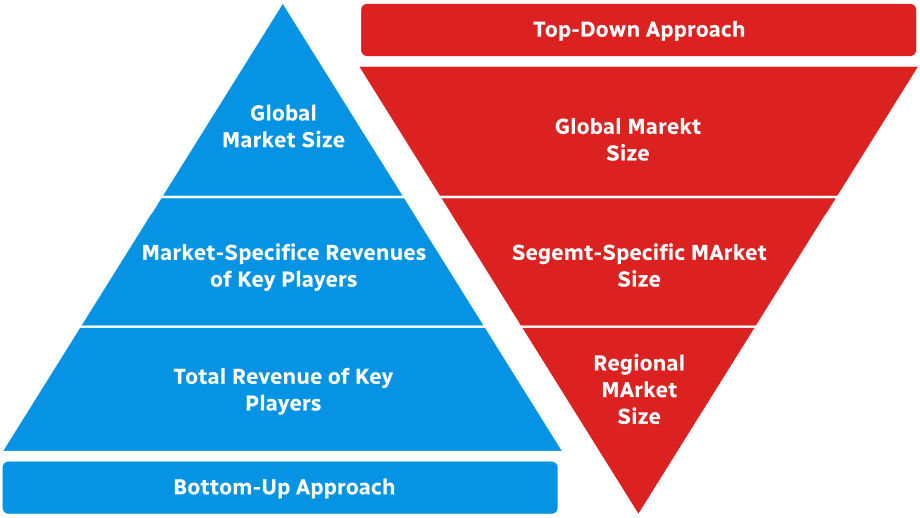
Primary Research
Secondary Research
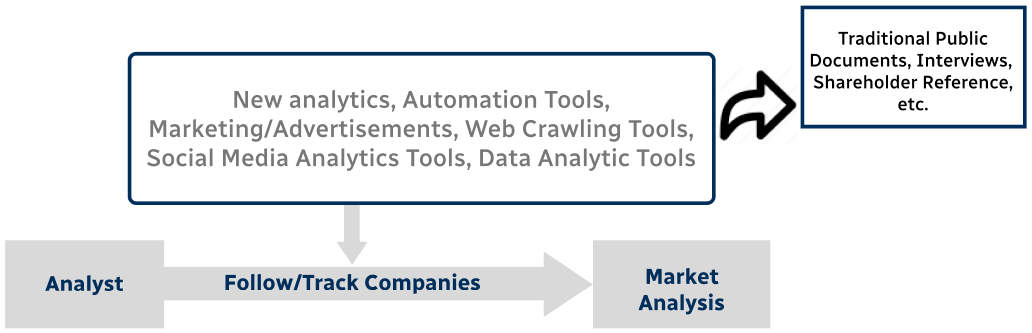
Involves using different sources of information in order to increase the validity of a study
These sources are likely to be stakeholders in a program - participants, other researchers, program staff, other community members, and so on.
Then we put all data in single framework & apply various statistical tools to find out the dynamic on the market.
During the analysis stage, feedback from the stakeholder groups would be compared to determine areas of agreement as well as areas of divergence
The projected CAGR is approximately 9%.
Key companies in the market include ClaimLeader, Ventiv Technology, TherapyNotes, SpeedySoft USA, Drchrono, Waystar, Meditab Software, Billing Dynamix, Claimable, HIPAAsuite, JW Software, Mitchell International, DataCare, PLEXIS Healthcare Systems, A1 Enterprise, RAM Technologies, NextGen Healthcare, .
The market segments include Type, Application.
The market size is estimated to be USD XXX N/A as of 2022.
N/A
N/A
N/A
N/A
Pricing options include single-user, multi-user, and enterprise licenses priced at USD 4480.00, USD 6720.00, and USD 8960.00 respectively.
The market size is provided in terms of value, measured in N/A.
Yes, the market keyword associated with the report is "Claim Processing Software," which aids in identifying and referencing the specific market segment covered.
The pricing options vary based on user requirements and access needs. Individual users may opt for single-user licenses, while businesses requiring broader access may choose multi-user or enterprise licenses for cost-effective access to the report.
While the report offers comprehensive insights, it's advisable to review the specific contents or supplementary materials provided to ascertain if additional resources or data are available.
To stay informed about further developments, trends, and reports in the Claim Processing Software, consider subscribing to industry newsletters, following relevant companies and organizations, or regularly checking reputable industry news sources and publications.